
| Home Forums |
|
|||||||
| Drugs and Drug Treatments ATG, Cyclosporine, Revlimid, Vidaza, Dacogen, ... |
 |
|
|
Thread Tools | Search this Thread |
|
#26
|
|||
|
|||
|
Thanks, Catherine!
It's great to see what it looks like. Thanks! Greg
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com |
|
#27
|
|||
|
|||
|
GREG
The technician who put my PICC line in at the NIH was just wonderful. I forget his name, but he was just great and made me feel so comfortable. I never had anything like that done before, and was, of course, nervous about it. But he had a great sense of humor which made me relaxed and he explained everything ahead of time. Like many of the wonderful employees there, he is of a foregin nationality.... maybe Latino, South American, or somewhere else; so if you get him, you're all set!!! Also, I love the guy I get down in Phlebotomy. He is from the West Indies. He is wonderful too! Always says when he puts your bands on your wrist "These are not gold or silver, but they are for you health, and that is worth more than anything"!.
the PICC line will dangle out of you upper arm. It will have 2 ports coming out of it, just in case one gets clogged up. That happens now and then and they will flush it out, but having 2 just makes it easier. They will either wrap in in that bandage like you get after your blood work in Phlebotomy, like a colored ace bandage, or in a white fabric type thing that basically keeps everything close to your arm. They will give you these clear, protective bandages to put over your arm, at the site of you picc line, that will stick onto your arm and cover the entire area, for when you shower. I had some redness at the site of my PICC line for a bit, but never enough of a concern for them to take it out and redo. They will check for infection at the site, so don't worry about it. Is tomorrow your 1st day........ EKG's etc? Best of luck to you. If you didn't take any reading material, visit the library in the building to get some. Keep us posted!
__________________
Dx. 6/08 with AA, then changed shortly thereafter to MDS. Campath trial at NIH March '09 and have been transfussion independent since June '09 |
|
#28
|
|||
|
|||
|
Hey Lisa!
Thanks for that great info. I love those sticky ace bandage things. Much kinder coming off. Tomorrow we do lots of heart stuff and check in to the inpatient clinic. Thanks! Greg
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com |
|
#29
|
|||
|
|||
|
Day 1 of the NIH Campath Trial
NIH Campath Trial Day 1 is nearly done, assuming nothing overly exciting happens between now and bedtime.
Here's the rundown: ECHOcardiogram first -- an ultrasound of your heart (for those who haven't had one). Technician was Russian by way of Israel. This is a very international place! Then EKG, plus outfitting with a Holter monitor for a 24 hour continuous EKG. You have to keep a little diary of activity with this, which was hard to remember to do, since we didn't really do much all day except walk around NIH. Seven vials of Blood contributed to the phlebotomists. Chest X-Ray. Consent forms with the Principal Investigator, Dr. Matthew Olnes, who let us know that they have applied to have their trial extended from the current 43 to as many as 80 patients, which will let them gather more data to publish while continuing to make this therapy available, until the accumulation of data can convince insurance companies that this is a viable therapy worthy of reimbursement, so lots of MDSers can benefit. Check in as inpatient. Interview (medical history) with the rotating Fellow who will be my primary Doc during the trial. Lunch. Boredom. So we walked around the facility, found the patient library, found the gym, could not find the wine bar, and eventually gave up and had dinner. That's about the size of it; more fun tomorrow when we get a PICC line and a little dose of Campath. Take care! Greg
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com |
|
#30
|
|||
|
|||
|
NIH
Dear Greg,
For those of us who might be considering a clinical trial we truly appreciate your minute by minute account. Boredom and no excitement is a good thing in the hospital. I wish you a very successful and uncompicated treatment. Heads up Marie
__________________
possible low to int-1 MDS with predominant thrombocytopenia, mild anemia, dx 7/08, in watch and wait mode |
|
#31
|
|||
|
|||
|
Greg,
Funny that you mention the consent forms. I remember the consent forms Ruth had had sign before her transplant. She had to acknowledge a huge list of unlikely but possible adverse conditions, side effects, and diseases, from A to Z, many of them at least as serious as MDS. It read like the index of the Physicians' Desk Reference! Thanks for taking us with you on your journey. Keep looking for the wine bar. |
|
#32
|
|||
|
|||
|
Oh, you got off easy! My final pre-transplant tests made me give up FOURTEEN vials!
 Quote:
Good luck tomorrow! The PICC line insertion isn't bad at all - just try to relax and you'll be fine. Mine gave me a bit of deep numbness in my arm for a few days, but after that, I didn't even know it was there. And when the nurse came to eventually take it out, it just pulled straight out and didn't need more than an average bandaid/plaster. I've seen more blood shaving my legs! 
__________________
36/F - 1984 SAA treated with ATG [complete remission until] Oct 08 - burst blood vessels in eyes and low platelets; Jan 09 - AA & hypo-MDS; July 09 - BMT (RIC MUD PSCT) July 10 - 10k for Anthony Nolan (1yr post BMT! 53:48) Sep 10 - Wedding!  I've run 5 marathons now!! (PB 3:30!) I've run 5 marathons now!! (PB 3:30!)
|
|
#33
|
|||
|
|||
|
We LIKE boredom during hospital stays. Hope there's a lot more of it!
__________________
Catherine, wife of Bruce age 75; diagnosed 6/10/11 with macrocytic anemia, neutropenia and mild thrombocytopenia; BMB suggesting emerging MDS. Copper deficient. Currently receiving procrit and neuopogen injections weekly, B12 dermal cream and injections, Transfusions ~ 5 weeks. |
|
#34
|
|||
|
|||
|
Day 2 of the NIH Campath Trial
Day 2 of the NIH Campath trial started at 5:30 am, when the mobile phlebotomist brought by his cart and left with thirteen tubes of my limited blood supply.
The early start wasn't too big a shock to the system, since I was already awake -- and had been all night, as a result of a last-minute roomy change that left me with an elderly "sundowner," who kept his television on all night and kept the nurses hopping with constant calls for more meds. That's one of the liabilities of the "semi-private room concept: there's no "semi" about the lack of privacy, not to mention the lack of dark and noise. It's tough for a country boy to sleep in the "urban" environment of a hospital ward. Ultimately, I plugged in my iPhone earbuds and hit shuffle for my extensive Van Morrison collection. That drowned out the TV, and I got about four hours of restless sleep. [I should say that I include this only in the interest of completeness and full disclosure, for the benefit of other folks who might be considering this or other trials, not as whining (or whinging). A man rescued from a shipwreck should not complain about the freshness of the beef on the schooner that plucked him from the briny deep.] I had an ambitious night nurse determined to get my PICC line placed early, instead of mid-morning, as scheduled. So it was over to the procedures area, which is run with a great deal of energy by a mustachioed charge nurse named "Mash." [Think Robin Williams as Adrian Cronauer in "Good Morning, Vietnam" and you'll have a good picture of the atmosphere.] After I refused Mash's demand for a five dollar tip for slipping me in early, he set me up with Elmer, the nurse who would be inserting my PICC line. Elmer was very thorough in describing the procedure -- and in warning me that he tended to hum and sing under his breath while he worked. I was treated to a medley of Filipino folks songs and a rousing hummed version of "Love is a Many Splendored Thing." Though the PICC Line insertion is typically a 20-minute job, mine took 90 minutes, because the catheter, or my circulatory system, was stubborn. Elmer used ultrasound to find the right vein on the inside of my upper arm, marked it, and measured the length over to my heart using a paper tape. After gowning up and numbing me with a little lidocaine, he started the insertion. All went very smoothly and we were about to do the chest X-ray to verify placement, when he decided to check the jugular vein in my neck with the ultrsound. Sure enough, the catheter had taken a wrong turn and would up in my neck. So, we pulled it out a ways, bent my head over, and tried again. After a couple of false starts, we found the vein that leads to my heart. Unfortunately, Elmer met with resistance three centimeters short of his target length for the catheter. Chest Xray confirmed we were short -- and showed that the tip of the catheter had acquired a little upwards bend. Another problem seemed to be that the vein in my arm had grown angry at all of the attention and showed its pique by spasming. Or, as Elmer said, "Your vein is biting me." After consultations with colleagues, we pulled the catheter back five centimeters and flushed it several times to straighten out the kink. Though we were still three centimeters short of the target measurement, another Xray showed an acceptable placement. We got some gauze, tape, and a transparent plastic bandage over the entire thing, as well as a wrap of that cool slightly sticky Ace bandage-like wrap they use here. That dressing is changed the next day, and then again a week later. A thick plastic barrier is placed over it for showering. (I think I should have shaved the hair from my arms before coming here! It would have been less painful.) 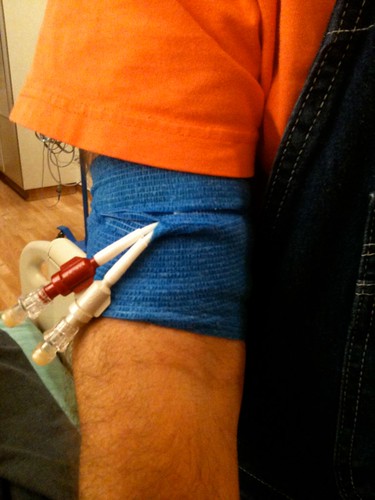 IMG_0479 by hankins.greg, on Flickr I have a two-port PICC, one for the meds and one for extracting blood, which the nurses can do with a very strange-looking plastic contraption. Among other pre-Campath events, we detached my 24-hour Holter monitor and its leads (maybe I should have shaved my chest as well). And, because I had recently had what I took to be a kidney stone attack, we went down to radiology for a kidney ultrsound, which found no stone. We are going to let that mystery be until I return home. I also had my first 500 mg Valtrex tablet in the morning. That's the anti-viral that I will be taking for many months to ward off infections. In the late afternoon the nurse hooked me up a bag of saline and the Campath. The latter bears warning labels about being a dangerous drug, and the nurse has to gown up before messing with it. After a little saline appetizer, the 1 mg test dose of Campath was started and administered over a one-hour time period. Even though this is a "test" dose, and far less than the 10 mg dose I will get for the next ten days, Dr. Olnes, the PI, told me the test dose kills off about 90 percent of the CD4 and CD8 T cells. Right at the end of the test dose, I began to get the chills and shakes (rigors). Warm blankets were piled on and demerol was offered. The demerol is strictly to control the rigors. I hate taking narcotics unless absolutely necessary, so I asked to wait a bit. The nurse and I agreed we'd give it 30 minutes and then re-evaluate. About five minutes before my grace period expired, the shakes stopped. I was utterly exhausted, from lack of sleep and the rigors, so I dozed off. Three or four hours later, the nurse, on a routine check, found I had a temp of 38.6C [101.5F]. This, she indicated, is to be expected with Campath. We lowered the room temp a bit (it had been raised during my chills) and took a couple of 325 mg Acetaminophen. I dozed off again, but another routine check in a couple of hours found my temp back to normal. And that was that. I slept all night like a baby. No hangover the next morning from Campath or the Demerol I didn't take.
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com Last edited by Greg H : Thu Nov 18, 2010 at 08:55 AM. Reason: Added photo |
|
#35
|
|||
|
|||
|
Bloggy, bloggy
Hi All!
If, for any reason, you prefer your reports on my NIH Campath trial with photos, you can feel free to hop on over to www.greghankins.com Where I, like Karen, have created a little blog. You'll find the updates and other news items under "The News." Take Care! Greg
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com |
|
#36
|
|||
|
|||
|
Nice blog, Greg. And it was nice getting to see your hospital ID!
 about the PICC line installation not going smoothly, about the PICC line installation not going smoothly,  about having a noisy roommate, and about having a noisy roommate, and  about having a good night's sleep and no unanticipated bad reaction to the Campath. Thanks so much for the very informative update. about having a good night's sleep and no unanticipated bad reaction to the Campath. Thanks so much for the very informative update.
__________________
Catherine, wife of Bruce age 75; diagnosed 6/10/11 with macrocytic anemia, neutropenia and mild thrombocytopenia; BMB suggesting emerging MDS. Copper deficient. Currently receiving procrit and neuopogen injections weekly, B12 dermal cream and injections, Transfusions ~ 5 weeks. |
|
#37
|
|||
|
|||
|
Good luck!
Greg~
Wishing you all the best! Safe travels and speedy recovery!
__________________
Cheri Age 54; dx Oct 2009 AML, induction chemo only;dx MDS July 2010,- PRBC transfusion dependent; Results BMB 8/4/11--- 6-8% blasts; Danazol 100 mg 3xday; quit Exjade/ GI distress; platelets holding 40's; Fluctuation in blasts in blood--Neupogen 3-4xweek; off Revlimid again! Procrit weekly |
|
#38
|
|||
|
|||
|
Hi - Thank you so much for your story -- I enjoy reading all the details and see the NIH has not changed all that much in 9 yrs. I had my ATG treatment there with Dr Sloan. Wonderful place that we can get the help that is needed. I hope you get some rest - maybe you will get a new roommate. They do change over it seems quickly. Best wishes to you. Keep up your wonderful humor thru all of this.
__________________
Susan Patient, 58, MDS, UPDATED 9/13 Now have RAEB-2, Firbrosis 3+, blasts 18% peripheral, 10 - 14% blasts marrow, chromosomes now T 1:21, trisonomy 16 and 1.- Match found ---10/10 -couldn't believe when I heard - Tentative day is 1/09th!!!! Admit date changed to 11/12. WOW - |
|
#39
|
|||
|
|||
|
Campath for AA, too.
Thank you Catherine, Susan, and Cheri for the kind words.
It's neat you were here, too, Susan! Dr. Sloand is actually the attending on the Campath Clinical Trial, with Dr. Olnes as the Principal Investigator. I'm not sure I have made clear in my past posts, being focused on my own disease, that there is a parallel Campath trial underway for folks with Aplastic Anemia. In fact a patient just down the hall is participating in that study. I don't believe any results have been published on that one, however. You can find it here: http://clinicaltrials.gov/ct2/show/NCT00195624 It appears to be for SAA folks who have failed to respond to or relapsed after ATG; the details are all on the page linked above. Take care! Greg
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com |
|
#40
|
|||
|
|||
|
Day 3 of the NIH Campath Trial
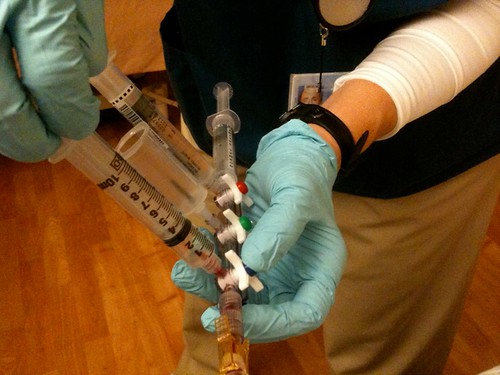 IMG_0483 by hankins.greg, on Flickr Day 3 of the NIH Campath trial began at 5:00 am, when I was awakened after a very long and restful sleep by the nurse for vitals and a blood draw. They use an amazing Rube Goldberg device to extract blood from the PICC Line and then flush the line. The nurse tells me it's called a "COBE Device." That's a photo of it above. The white knobs control which syringes, etc. are connected to the PICC line at any time. The nurse makes sure only the first syringe is "live" and extracts the appropriate amount of blood into the syringe. She then twists the knobs to cut off flow from the patient and turn on flow to the second station in line, which is like the typical gizmo used to draw blood into vials. She inserts a vial, and the blood passes from the syringe into the vial. Once the tubes are all full, she uses the tube on the end to flush the line. The first vial of blood is a discard; after that, it's whatever the doctor ordered. Unlike Day 2, when thirteen tubes were extracted for research, this morning it was only two tubes. We're doing a CBC with Diff each day, as well as a "Chem 20 Panel," which has all the liver and kidney function stuff. And there's also a breakdown of various lymphocytes, including CD3, CD4, CD8, CD19, and Natural Killer cells. We are past all the screening and testing now, so, after the blood draw, the morning is spent getting ready to have Campath, which happens around 10:00 am, and the afternoon is spent recovering. Impact on counts The day nurse kindly printed out my labs, which were pretty interesting. The most amazing result was the lymphocyte count. These are the guys we are trying to kill off to stop the war in my bone marrow. Prior to the 1 MG test dose, the count was 1.15K/uL. The morning after the test dose, the count had dropped to 0.18 K/uL. A single 1 mg dose of Campath knocked out 84% of my lymphocytes. And I'll have 101 mg by the time we are done. The other impact included an Hgb drop from 10.3 to 9.5 and a platelet drop from 69 to 52. The test dose basically didn't touch the neutrophils, however, with 1.49 before and 1.47 after. These will probably take a hit from the full doses, but we want them to stay as high as possible -- out of serious neutropenic territory. First big dose The first 10 mg dose of Campath started at around 10:00 am and was administered over a two hour period. About three quarters of the way through, the chills started, followed quickly by the rigors. The latter were more severe this time and more continuous. After about ten or fifteen minutes of that, I gave up and went for the demerol. It was probably a good thing. My back was aching all evening -- likely from the tensing and shaking involved in the rigors. All three of my docs -- the Fellow who is my main doc on the floor, the attending who runs the Fellows, and Dr. Olnes, the PI -- all scolded me for doing without the demerol with the trial dose -- as did the trial coordinating nurse, Barbara Weinstein. The 25 mg of demerol (a half-dose) took less than five minutes to quiet everything down. Just about the time the dose finished, my fever began to climb, hitting close to 104 before coming back down over a period of three or four hours. Oddly, I had a huge allergy attack later on in the afternoon: Sinus congestion followed by nose running like a faucet. My wife Marcy had gone to grab some lunch at the cafeteria on Level B1 of the older part of the Clinical Center -- the Magnuson building. She was also experiencing some allergy symptoms when she returned. After supper, at just about the time my sniffles had stopped, she took me back down to the cafeteria, so I'd know how to find it. I immediately began a sneezing fit (I recall that Melissa had a sneezing fit with Campath!), and my nose ran all evening, even after the doc prescribed Zertec. I honestly don't know whether there is some allergen lurking down on Level B1 or if it was Campath-related, but I tend to think the former, since Marcy was affected as well. There was little other excitement on Day 2. I managed a shower without getting my PICC dressing wet -- they use a thick plastic barrier called AquaGuard. And the dressing was changed. The new one is good for a week, if I don't get it wet. The second 10mg dose is tomorrow and I expect more rigors and fever. But, with luck, that may begin to tail off on Day 3.
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com |
|
#41
|
|||
|
|||
|
Thanks for the very informative (and entertaining) rundown! I've never seen those COBE devices before, either! How cool and streamlined...
Quote:
If if makes you feel any better, my reaction the first night was the most severe, and it tailed off considerably with each dose. Fingers crossed for your next doses!
__________________
36/F - 1984 SAA treated with ATG [complete remission until] Oct 08 - burst blood vessels in eyes and low platelets; Jan 09 - AA & hypo-MDS; July 09 - BMT (RIC MUD PSCT) July 10 - 10k for Anthony Nolan (1yr post BMT! 53:48) Sep 10 - Wedding!  I've run 5 marathons now!! (PB 3:30!) I've run 5 marathons now!! (PB 3:30!)
|
|
#42
|
|||
|
|||
|
So glad you made it through the first big dose of Campath (relatively) unscathed. And very glad the demerol is helping the rigors. Thank you again for all the trouble you're taking to document this.
__________________
Catherine, wife of Bruce age 75; diagnosed 6/10/11 with macrocytic anemia, neutropenia and mild thrombocytopenia; BMB suggesting emerging MDS. Copper deficient. Currently receiving procrit and neuopogen injections weekly, B12 dermal cream and injections, Transfusions ~ 5 weeks. |
|
#43
|
|||
|
|||
|
Greg,
Sounds like you're doing very well (aside from the daymare insertion of the picc line)! Love your blog, especially the photodocumentary approach. Thanks for keeping us posted. Sending you good thoughts for continued success. Karen
__________________
Karen, age 62, dx MDS RAEB-2 1/8/10: pancytopenia WBC 2.7k/Hgb 7.4/Hct 22.1/Plt 19k; complex cytogenetics -3,del(5)(q14q33),-6,+8,+mar,17% blasts. MUD BMT Johns Hopkins 11/30/10. Dx tongue cancer 8/31/12. ok now. blog mausmarrow.com |
|
#44
|
|||
|
|||
|
Greg
Keep letting us know how this is going for you. Glad you are able to handle things and keep the humor coming. Best to you -
__________________
Susan Patient, 58, MDS, UPDATED 9/13 Now have RAEB-2, Firbrosis 3+, blasts 18% peripheral, 10 - 14% blasts marrow, chromosomes now T 1:21, trisonomy 16 and 1.- Match found ---10/10 -couldn't believe when I heard - Tentative day is 1/09th!!!! Admit date changed to 11/12. WOW - |
|
#45
|
|||
|
|||
|
NIH Campath Trial Day 4
Day 4 of the Campath Trial at the National Institutes of Health was the second day of a full 10 mg dose of the drug.
We started the day at 5:00 am, contributing a couple more vials of blood to the Phlebotomy lab. I finished up yesterday's report and ordered breakfast while waiting for my Fellow, Dr. Klost, to make his 8:00 am appearance.  IMG_0494 by hankins.greg, on Flickr Lisa Z mentioned in a post on this thread that the NIH kitchen allows you to order any time of the day. Hours are from 6:30 am to 6:30 pm, and you have a one-page breakfast menu and a two page lunch dinner menu, plus page of liquids. They switched to a Fall menu this morning. Many of the items stayed the same from the Summer menu, but some changed. If you're on a special diet, the room service operator is aware of that and won't be able to get you certain items. If you are "regular," like me, you can as much as you want, whenever you want. The food is in fact pretty good, though quality varies across the menu, so you have to experiment a little to find the stuff you like. I like omelettes with spinach, mushrooms, and swiss cheese, but your mileage may vary. It takes about 45 minutes from ordering to get the food delivered to your room. There's an Au Bon Pain down in the first floor lobby if you like a decent cup of coffee in the mornings. They open at 7:00 am, but not on weekends. There are two cafeterias and a convenience store that your caregiver/visitors can use for nourishment. Big Dose 2 -- Waiting for the rigors. After Valtrex, Tylenol, and Benedryl at 9:30 am. We started the two-hour Campath drip at 10:15 and I held my breath for two hours waiting for the rigors to start. One hour, nothing; 1:30, nothing; 1:45, nothing. Two hours, nothing. No rigors! Two hours after the Campath, I got the chills, but the shakes never appeared. Warm blankets worked for the chills. My fever started to spike around 3:30 pm, 38.1C or 100.5F. Eating ice took that down without Tylenol. It came and went during the night, but never higher than 100F. And that, was that.
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com |
|
#46
|
|||
|
|||
|
Quote:
Of all the medical equipment and supplies in our hospital, we thought most highly of one in particular: the blanket-warming machine. Whether a patient was shivering during treatment or merely a little chilly while waiting around, a heated blanket brought by the nurse was so very welcome. When it comes to patient comfort, it's the #1 treatment! |
|
#47
|
|||
|
|||
|
Quote:
__________________
Catherine, wife of Bruce age 75; diagnosed 6/10/11 with macrocytic anemia, neutropenia and mild thrombocytopenia; BMB suggesting emerging MDS. Copper deficient. Currently receiving procrit and neuopogen injections weekly, B12 dermal cream and injections, Transfusions ~ 5 weeks. |
|
#48
|
|||
|
|||
|
Greg-
Hi Greg-, Sorry I didn't get around to the forum until today..... busy week here at home. Sounds like most of the side effects that one can have, you are experiencing. Makes my experience almost sound boring. The only problems I had were the rigors following first 2 doses, but I took the Demerol right away, and yeah, you gotta love those warm blankets. They are the best.
Mash, yes, he was the one who put in my PICC line. He gave me the $5 tip joke as well. Sorry experience with that step of the process wasn't so easy. Interesting........ when I was on the trial, Dr. Sloand was PI and Dr. Olnes was attending. Now, they have switched. Dr. Olnes is who I always e-mail if I have any questions. Even now, 1.5 years after the treatment, he is always willing to answer my questions promptly and thoroughly. You are in great hands! So, sounds like all in all, you are doing OK. Too bad you had to have a roommate. I had my own room, which was very nice. My husband spent the night .... each night, and when he ran home for the weekend, my mom came to stay with me. But, in some ways, it might be good for you. You have 24/7 "company" as well. I'm sure the rest of your stay will get easier and easier as each day goes by. Keep us posted. Have a Happy Thanksgiving. I'm sure they'll have a special menu item on Thanksgiving. Wishing you the best, Lisa
__________________
Dx. 6/08 with AA, then changed shortly thereafter to MDS. Campath trial at NIH March '09 and have been transfussion independent since June '09 |
|
#49
|
|||
|
|||
|
Cleared for the gym!
Hey guys!
Thanks for the good wishes. Catherine, you will be pleased to know I have been approved for gym duty. I can use the treadmill or stationery bike, but no upper body training, since I have the PICC Line in. Neil and Lisa Z, I hear you on the blanket warmers. A fantastic thing when you are chilled and way better than a pharmaceutical solution. I've had some other observation on hospital design/operations during my stay, which you'll find at the end of my post on Day 5, coming up. I'll be interested in your thoughts. Take care! Greg
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com |
|
#50
|
|||
|
|||
|
NIH Campath Trial Day 5
Day 5 of the NIH Campath trial is going to result in a pretty boring report:
No chills. No shakes. No fever. In other words, things are going just about according to plan. Thursday was my third full dose of the drug, and my body has evidently reconciled itself to the fact that I will be pumping poison into it on a regular basis for a while. The counts are looking pretty good. The lymphocytes, our target, have taken another blow, and are now down to 0.02K/uL (i.e., 20 per microliter). Meanwhile, the neutrophils are putting up a good fight and managed to stay over 1,000, at 1,200 per uL. That's still a comfortable distance from the 500 threshold that will put me on Cipro and a neutropenic diet. After taking some big hits, platelets only dropped from 35,000 to 30,000 today; transfusion target is 10,000. Hgb is at 8.2, portending an RBC transfusion in the next couple of days -- to be expected in this protocol. Why don't patients talk with each other? Since my results are pleasantly predictable, let me share some thoughts on another aspect of this place. One of the really neat things about the Clinical Center at NIH is the number of bright open spaces left throughout newer portion of the building -- the Hatfield Center, completed in 2004. Those sun-filled lobbies are everywhere, with all manner of comfortable, upholstered seating -- from sofas to side chairs and recliners. There are even study carrels like those in a college library. There are also plenty of well-appointed small waiting rooms, big enough for four or five folks to have some privacy.  DSCN4790 by hankins.greg, on Flickr It seems to be part of a grand design to get patients up, dressed, and out of their standard-issue hospital rooms, meeting and chatting with other patients -- thereby accelerating the healing process. It's a wonderful idea . . . which doesn't really seem to work. Most of that upholstered furniture seems to remain empty most of the time. Why is that? Some patients, of course, are just too sick to leave their rooms. They feel seriously crummy and really do want to lie in bed all day. In the hematology/oncology unit, some folks are recently neutropenic, and have been made paranoid (perhaps usefully so) by the nurse's explanation of what that means. So they are cowering in their rooms until they get over the shock and can face the world in a face mask. But a lot of the problem is that the day-to-day operational mechanics of life in the hospital haven't caught up with the architect's vision of that life. When it's time to check vitals or administer meds, nurses show up at your room and expect to find you there. When the doctor has news to impart or wants to check up on you, he drops by the room and expects to find you there.  DSCN4795 by hankins.greg, on Flickr If you want to speak with your nurse, typically your only option is to press a button on a device in your room in order to speak with a a disembodied voice who will call your nurse on a phone the nurse has in his pocket. You cannot, however, call that phone in your nurse's pocket directly. If you want to speak with your doctor, you can either wait in your room 'til she comes around; or you can push the button to tell the disembodied voice to fetch your nurse and then tell him that you'd like to speak with the doctor so that the nurse can then work through whatever system he has (typically mysterious to the patient) to contact the doctor. Often that system seems to amount to waiting until the nurse happens to see the doctor on the floor, though the nurses here at the Clinical Center can use a text paging service to send the doc some detailed info about who wants to see him and why. The doc will then drop by your room at some random time, expecting to find you there. In short, if you want medical care, you have to stay in your room. The net effect of all this is to keep patients in their rooms, instead of out in the nice comfortable lobby furniture that the architects felt would help keep patient's lives more normal, helping them heal more quickly. What's the solution? I don't know for sure, but a big step forward would be to put the pagers on the patients. The devices don't have to be fancy; they can use the same sort of system now used in restaurants, so folks waiting for a table don't have to stand around clogging up the foyer. Put a button by the door for the nurse or doc to press. That sets off the pager; and the patient knows, when the pager goes off, that she has five minutes to be back at the room. Even better, get the patient's cellphone number, crank it into the unit database, and let the nurse or doctor call the patient to answer a question or set up an appointment: "Hi Mr. Hankins, this is Dr. Klotz. I understand you wanted to see me. I'll drop by your room about 3:30." I know most hospitals don't want you to use your cellphone, but everyone -- including the staff -- seems to do it anyway. The NIH Clinical Center staff are actually pretty good at doing some things to make patients' lives more predictable -- like letting the patient know about the day's schedule in the morning, having a reliable schedule for rounds, and using text paging for the docs. But all of that hasn't managed to get most patients out in the lobbies. If the lobbies make sense, it makes sense to take the next step and make it possible for patients to use them while at the same time getting good medical care. What do y'all think?
__________________
Greg, 59, dx MDS RCMD Int-1 03/10, 8+ & Dup1(q21q31). NIH Campath 11/2010. Non-responder. Tiny telomeres. TERT mutation. Danazol at NIH 12/11. TX independent 7/12. Pancreatitis 4/15. 15% blasts 4/16. DX RAEB-2. Beginning Vidaza to prep for MUD STC. Check out my blog at www.greghankins.com Last edited by Greg H : Sun Nov 21, 2010 at 12:50 PM. Reason: Added Photos |
 |
| Thread Tools | Search this Thread |
|
|
 Similar Threads
Similar Threads
|
||||
| Thread | Thread Starter | Forum | Replies | Last Post |
| Pilot study of Alemtuzumab (Campath) at NIH | Barbara2007 | Clinical Trials | 9 | Thu May 5, 2022 12:38 AM |
| New Promacta (Eltrombopag) Clinical Trial at NIH | Sally C | Clinical Trials | 73 | Sun Dec 30, 2018 05:52 AM |
| NIH Trial - Plt Count Level Feedback/Experience | disco3md | AA | 1 | Wed Jun 28, 2017 01:08 PM |
| NIH Trial (Eltrombopag & Cyclosporine) | disco3md | Clinical Trials | 0 | Mon Jun 26, 2017 05:02 PM |
| Subcutaneous Campath Trial | Nadia T | Clinical Trials | 3 | Fri Dec 20, 2013 09:06 PM |